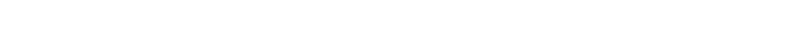UW Health nurses have authorized a three-day strike next month, ratcheting up their bid to regain a union lost because of a 2011 state law, amid what organizers call a “dangerous crisis of understaffing” made worse by the COVID-19 pandemic.
Nurses voted Wednesday to strike from 7 a.m. Sept. 13 to 7 a.m. Sept. 16, but said the UW Hospital Board could avoid the strike by recognizing the union. Otherwise, nurses will provide a 10-day notice of the strike so administrators can prepare, as required by labor law.
“UW nurses have been struggling with a dangerous crisis of understaffing, turnover, cuts, exhaustion and burnout, which has been aggravated by the pandemic and puts patient care at risk,” SEIU Healthcare Wisconsin, the union trying to organize the unit, said in a statement Thursday. “They are calling for a union voice on the job so they can solve these critical problems and advocate for their patients, community, families and themselves.”
People are also reading…
In a statement, UW Health called the decision to strike “disappointing” and said a strike would be “unpleasant for patients and for our staff but we will get through it.”
UW Health said the union could petition the state for recognition, which would “move us closer to getting a definitive answer from the courts on whether UW Health can legally recognize and bargain with a union.”
Compensation for nurses is “among the best in the region,” staffing ratios are “among the best in the nation,” and the nursing turnover rate is roughly half the national average, UW Health said.
“No national advocacy campaign can take away the fact that UW Health is a great place to work with the highest quality care in Wisconsin,” the statement said.
Act 10 aftermath
Former Republican Gov. Scott Walker’s signature legislation, Act 10, banned collective bargaining for public workers except for cost-of-living pay increases. At the time, UW Hospital administrators said the law abolished unions at the hospital even though they didn’t seek that action. In 2014, when a contract for about 2,000 nurses and therapists represented by SEIU expired, they lost the union.
In December 2019, shortly before the pandemic began, nurses announced they were restarting the union and asked the UW Hospital Board to voluntarily recognize it. The board and hospital leaders have repeatedly said the law doesn’t allow them to recognize and bargain with the union.
Unlike other public employees affected by Act 10, UW Hospital workers are not state or municipal employees. When the hospital became a public authority separate from the university in 1996, it acquired its own special status. How Act 10 and other laws apply to that status has been the subject of various legal memos.
After two memos last year from the nonpartisan Wisconsin Legislative Council appeared to reach different conclusions, Democratic Attorney General Josh Kaul in June said the hospital can contract with its employees and set their terms of employment through a voluntary collective bargaining process. Kaul’s nonbinding opinion came at the request of Democratic Gov. Tony Evers.
On Thursday, UW Health’s statement said: “The Attorney General has said he believes we can, but by his own admission states that his opinion is not law and that only the courts or the legislature can provide a conclusive answer.”
Amid the legal debate, nurses have drawn attention to what they say are difficult working conditions that threaten patient safety as the COVID-19 pandemic continues. In January, SEIU Healthcare Wisconsin said it gave UW Health CEO Dr. Alan Kaplan more than 1,500 cards signed by nurses supporting a union. SEIU says 2,600 nurses at UW Hospital would be in the bargaining unit.
The union on Thursday declined to specify how many nurses voted to strike, only saying it was “hundreds.”
SEIU also represents nurses at UnityPoint Health-Meriter in Madison. Nurses at SSM Health St. Mary’s Hospital in Madison don’t have a union.
Law and leverage
State and federal law allows workers to strike even if they’re not part of a recognized union, said Alexia Kulwiec, an associate professor of labor education at UW-Madison and co-chair of the university’s School for Workers.
“Employees have the right to engage in concerted activity,” such as protests and strikes, Kulwiec said. “You don’t have to be in a union setting.”
While the nationwide shortage of nurses could empower UW Health nurses in their effort to strike, large hospitals typically go to considerable lengths to counter such actions, said Steve Striffler, director of the Labor Resource Center at the University of Massachusetts-Boston.
“Intuitively, (the labor shortage) should translate into increased leverage for workers and particularly workers in hospitals,” Striffler said. “But it doesn’t lead administrators or owners of these hospitals to lay down and let themselves get walked over. It’s still a very contentious set of labor negotiations.”
In Worcester, Massachusetts, nurses at St. Vincent Hospital, owned by the large, Dallas-based company Tenet Healthcare, last year went on strike for nine months, with the hospital bringing in replacement workers.
Unlike Tenet, UW Health doesn’t have numerous facilities in many states. Along with UW Hospital and related facilities, it owns SwedishAmerican Health System in Rockford, Illinois. Striffler said that could make it harder for UW to find backup staff.
“The question is, given the (nursing) shortage, whether the University of Wisconsin Hospital can pull that off or not,” he said.
For a short strike like that authorized by the UW Health nurses, employers typically rely mostly on managers and supervisors to fill in, Kulwiec said.
National trend
Nurses around the country have vowed to strike, including this month in Minnesota, saying hospitals are understaffed and nurses are overworked.
The federal Bureau of Labor Statistics, which only tracks strikes involving 1,000 or more workers, said there were 16 such strikes last year, four of which involved unions representing health care workers.
At least seven health care organizations in California have had workers vote to strike this year, with most of the strikes averted through negotiation, according to the news outlet Healthcare Dive.
Even before the pandemic, Wisconsin faced a projected shortage of about 11,600 nurses by 2030 as an aging population is expected to need more care, according to a state Department of Workforce Development report in May 2020.
As the pandemic intensified last year, 10.8% of hospital nursing jobs became vacant, the highest level since 2005, according to a Wisconsin Hospital Association report in March.
“We’re striking to put an end to the vicious cycle of understaffing and burnout and to win a union voice so we can protect the health of our patients and each other,” Tami Burns, a registered nurse who has worked at UW Health since 2017, said in a statement.
Burns said she and her colleagues have seen many patient deaths during the pandemic. “Compounding this brutal experience has been the almost total lack of support and resources from the UW Health administration. We’ve been suffering from extreme short staffing and cuts, and there’s a mass exodus of our talented nurses. Many of the nurses who’ve left have been medically diagnosed with PTSD, including myself.”
Colin Gillis, a registered nurse at UW Health for five years, said in a statement that nurses at the bedside need to be involved in decision-making about patient care. “Turnover and understaffing force us to make gut wrenching decisions: Do I stay with a patient who’s medically unstable, or do I leave to give medicine to someone in dire pain?”
State Journal reporter Jeff Richgels contributed to this report.
Fave 5: Reporter David Wahlberg picks his top stories of 2021
COVID-19 dominated my year again as the State Journal’s health reporter, except for June and July, when it seemed we might overcome it. Vaccinations and variants were new angles this year. I also covered continuing deaths from the pandemic and challenges for health care workers.
During the summer dip in coronavirus activity, I wrote about a little-known hereditary disorder tied to several cancers, for which Fitchburg-based Promega Corp. has developed related testing.
This fall, I spent much of my time working on a three-day series about newborn screening, focusing on how the testing varies among states. If you were born since the mid-1960s or had a child since then, you’ve almost certainly taken part in this screening, which looks for rare diseases for which prompt treatment can prevent death or disability.
I love transplant stories. Dr. Matt Wolff had quite a backstory to his heart-kidney transplant.
In February, I wrote six more vignettes about people who died from COVID-19.
Little-known Lynch syndrome is more common than BRCA mutations for breast cancer.
In September, I visited the COVID-19 unit at St. Mary's. These dedicated workers are tired.
I spent much of the fall looking into the unequal practice of newborn screening among states.